
HOW TO CLASSIFY PAEDIATRIC LOW VISION?
Lea Hyvärinen, MD
When we discus a classification we should, as the first question, ask ourselves what the classification is used for. Classification of paediatric low vision is needed to describe the infants and the children who are entitled to receive early intervention and special education because of their visual or multiple disabilities. Since more than half of visually impaired children have several impairments that affect their activities, the effect of all impairments is important to assess and classify. It would be of great importance to have a classification reflecting present understanding of the degree and type of visual disability that requires special education and services.
Preceding the ICEVH Conference in Bangkok in 1992, an expert group was called to a meeting by WHO and the ICEVH to discuss paediatric low vision. That meeting resulted in a statement with two important details that make the definition of paediatric low vision different from the WHO classification of visual impairment in adult persons:
it included other visual functions than visual acuity and visual field and
it included the statement "This working definition is solely designed for reporting purposes and SHOULD NOT be used for eligibility for services". The Bangkok Recommendation thus is related to reporting to WHO, it does not define disability. This recommendation is not known in many countries and children are therefore assessed as if they were small adults even in infancy.
The present visual acuity values and visual field recordings, which are used for classification, do not always correctly depict visual function even in older children. I would like to show a few examples of problems caused by the present classification of visual impairments.
 In Scandinavia we have a mild form of retinoschisis with changes in the foveal structures of the retina causing decrease in visual acuity below 0.3 (equal to 3/10, 6/18 or 20/60) but not affecting other visual functions. When we see these boys among their peers, it is difficult to notice any inferiority in their functions. The boy, who is shown in this video, was one of our best young ice hockey players, yet would be classified as visually impaired because of low central visual acuity. However, since all other visual functions are normal, his visual performance is normal.
In Scandinavia we have a mild form of retinoschisis with changes in the foveal structures of the retina causing decrease in visual acuity below 0.3 (equal to 3/10, 6/18 or 20/60) but not affecting other visual functions. When we see these boys among their peers, it is difficult to notice any inferiority in their functions. The boy, who is shown in this video, was one of our best young ice hockey players, yet would be classified as visually impaired because of low central visual acuity. However, since all other visual functions are normal, his visual performance is normal.


Similarly another younger boy, shown in the video, with a mild case of retinoschisis functions like a normally sighted child when learning his alphabet with a computer game, when constructing a complicated space ship of Legos and in all other play situations. However, in other children, retinoschisis may cause more severe loss of vision.
 Youngsters with Usher Syndrome, retinitis pigmentosa and deafness, are often classified as deaf, normally sighted if their visual acuity is normal, even if they may have problems with night vision and photophobia, and disturbances in the image quality. When they tested different filter lenses during a winter weekend gathering; healthy, active youngsters with dual sensory impairment, you could not tell who are the youngsters with Usher Syndrome and who are their siblings. You would notice their visual problems if they did not have their special filter lenses on a bright sunny day. They rarely describe the disturbing light phenomena in their visual field if you don't ask about them because these floating "sausages" may be taken as signs of insanity.
Youngsters with Usher Syndrome, retinitis pigmentosa and deafness, are often classified as deaf, normally sighted if their visual acuity is normal, even if they may have problems with night vision and photophobia, and disturbances in the image quality. When they tested different filter lenses during a winter weekend gathering; healthy, active youngsters with dual sensory impairment, you could not tell who are the youngsters with Usher Syndrome and who are their siblings. You would notice their visual problems if they did not have their special filter lenses on a bright sunny day. They rarely describe the disturbing light phenomena in their visual field if you don't ask about them because these floating "sausages" may be taken as signs of insanity.
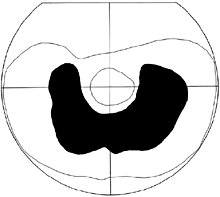
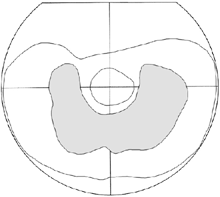
Quite recently I have become aware of one more weakness in our assessment techniques when assessing retinitis pigmentosa. A teen-age deaf boy had a large, nearly complete "absolute" ring scotoma in Goldmann visual fields ("absolute" meaning that there was no response). He had been told not to drive his bike any more. I confirmed the finding but heard that this boy was the best goalkeeper in ice hockey in the junior league playing with hearing, normally sighted peers. We therefore measured flicker sensitivity in the area of the "absolute" scotoma, and he responded in all parts of the scotoma, which thus is not absolute but only relative. There is motion perception, which is not measured in the usual clinical examination and which is the visual function used in ice hockey.
It is an important problem that the two measurements that are now used for classification of low vision, visual acuity and visual field, do not depict visual disability in a number of cases.
When we make a decision on special education it should consider all areas of visual functioning. A child who needs special skills in education of academic subjects, most often needs special education also in other skills, in daily living skills, orientation and mobility and communication.
To someone who has worked with visually impaired children it is rather obvious whether a child needs to use techniques typical to blind persons or techniques typical to low vision or whether the child uses regular techniques of normally sighted children in different tasks. The prerequisite is that the evaluator knows the differences in techniques and can observe when the child switches from one technique to another. As you know, visually impaired children use different techniques in different tasks depending on the type of vision loss.
A child with central scotoma and low visual acuity may need very high magnification, even CCTV to read, or prefers Braille and talking books when longer texts need to be read. These children may have no problems in orientation and moving in known places where they thus use techniques typical to normally sighted but may have problems in unknown places. So there is variation from techniques typical to blind persons or those typical to severely visually impaired in sustained near vision tasks to techniques typical to normally sighted in orientation in known environments.
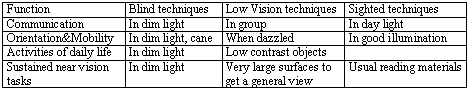
If we assess the use of the techniques in each of the four main functional areas, communication, orientation and mobility, daily living skills and sustained near vision tasks like reading and writing, we get useful information for planning special education. If we describe the findings in a diagram (Hyvärinen 1999), we can fine-tune the description by using lines to depict variation in the use of the different techniques or describe them as a function of luminance if the child has poor night vision (Table 1.).
Table 1.
Children with Retinitis pigmentosa are a big group of children with good visual acuity. Another growing group are children with vision loss due to brain damage. These children with CVI, Cortical Visual Impairment, as it is often called, or Cerebral Visual Dysfunction or Disability, often have normal or near normal visual acuity with single symbol tests but poor acuity with crowded symbol tests. A child with visual acuity 0.8, equal to 8/10, 6/9 or 20/25, may need to use CCTV. Children with CVD may have difficulties in:
- recognising people
- recognising facial expressions
- perception of motion
- perception of objects standing still
- perception of object-background
- eye-hand co-ordination and
- orientation in egocentric and/or allocentric space
These visual functions can be tested in quite young and even severely disabled children. As an example I showed testing of a 6 years old boy. We knew that he recognised people two weeks after he became conscious after severe encephalitis, but which details he used to recognise, was not known.
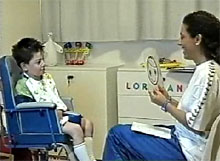

First test was with Hiding Heidi to measure whether he could see facial features at low contrast. That he did. Next we tested whether he could perceive and recognise different basic expressions using matching. That was successful, too. The boy used pointing with gaze as the mode of answering.

His fixation was somewhat unsteady but he could voluntarily shift his gaze. With the LEA Rectangles we proved that he could compare lengths at near distances and could select the correct length. This function is close to visual acuity so that was measured next. Because of communication difficulties only single symbol test was used during this first testing. His visual acuity was found to be 0.5, equal to 5/10, 6/12, 20/40. His visual acuity and other visual functions are likely to improve so all these tests and visual acuity as line test and with crowded symbols will be measured at regular intervals.
Although we can describe the techniques used and thus the needs of special education, it is not enough for administrators and lawyers. They want to have numbers in the classification. Since we have three different techniques that can be used, and four different main functional areas, we can depict the functional situation with one number by giving points to the three different techniques. It is possible to give 1 point to blind techniques, 2 points to low vision techniques and 3 points to sighted techniques (Hyvärinen 2000). Special teachers prefer giving 3 points to blind techniques, 2 to low vision techniques and 1 point to techniques typical to normally sighted. The variation is then between 12 and 4 points:
12 points in case of functional blindness,
11-10 points for severe low vision,
9-8 for moderate low vision,
7-6 for mild low vision,
5 for near normal and
4 for normal sighted functions.
By combining this numeric classification and the description of variation as a table, we are able to give clear information about the degree of impairment and the type and degree of disability, so that the need for services can be understood. This classification does not tell which kind of disability and need of services the child has. If a child has loss of only one function, for example face blindness, inability to recognise people by their facial features, he would get only 3 points and thus would be classified as normally sighted, which would be wrong. Face blindness is a severe loss of visual functioning in communication situations. Use of common sense should be required in all assessments.
Assessment and classification of young infants needs to consider all areas of development so that proper techniques are taught to the infant. As you know, severely visually impaired infants develop their communication, motor skills, spatial concepts, object permanence, language and social skills different from sighted children because their experiences of the environment and other people are different from those of infants with normal sight. So all developmental areas need to be considered separately. When this is done, the need of special therapies can be defined.
I believe that these few examples have demonstrated to you that we need a classification that is based on techniques used by the child. It is possible to use a classification based on functions and techniques used in these functions, to chose a few main activities, and as a result have a numeric scale of disability. How the scale is structured in detail, should be decided by a group of experts in the field of education and medicine. Individual specific needs have still to be considered in each case. Our goal is to have a classification that is based on functional abilities and that helps each visually impaired child to receive proper early intervention and special education.
Reference:
Hyvärinen L. Assessment of Low Vision for Educational Purposes and Early Intervention, Part I.
Hyvärinen L. Understanding Paediatric Low Vision. Keynote speech at VISION99, New York.
The videos shown during this presentation are on my CD "LH Materials".
[ Back ]
Cracow-ICEVI2000