STRUCTURE OF THE EYE
The eye is a little ball with a thin case around it. Inside the ball there is jelly-like fluid. The diameter of the eye is 2.5cm or one inch; the eye weighs 7g or 1/4 ounce.
Sclera and Cornea
The white part of the eye is called the sclera. Healthy corneas have no blood vessels or discolorations. Many diseases, however, cause grey patches (opacities) to appear in cornea. Sometimes vessels grow into the cornea. Vision becomes blurred when the cornea is cloudy. Contact lenses sometimes irritate the cornea. Contact lenses may make vessels to grow into cornea.
The cornea is the clear membrane in the front of the eye over the black circle (pupil) and colored ring (iris). The cornea has numerous nerve endings. Therefore even slight irritations such as a hair touching the cornea may hurt. Also if a piece of dirt gets under the eye lid and scratches the cornea it is very painful. If the cornea becomes dry the surface (called epithelium) shrinks a little and the nerve endings are stretched. This causes a pain that often is as if a pin was stuck into the eye. The pain disappears if one closes the eye for a few seconds.
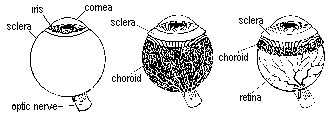
Fig.1. The most important structures of the eye
Eye doctors and many schools have a three dimensional model of the eye. In the model you can see the different parts of the eye better than in a picture. You can ask the doctor to show you which part of the eye he means.
Corneal transplant
If the cornea has become cloudy, it is often possible to remove the cloudy central part of the cornea and replace it with a piece of clear cornea (a corneal transplant). The clear piece of cornea is taken from a cadaver eye. Eye banks collect eyes for corneal transplantation. Persons who want to donate their eyes carry a special card. When such a person dies the eyes are removed and sent to the eye bank.
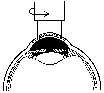
|
Fig.2. The central part of the cloudy cornea is removed with a small circular trephane. The clear corneal graft (transplant) is removed from the donated eye and sewn with very fine thread in the center of the patient's damaged cornea. |
Sometimes the clear graft becomes cloudy if the patient's body does not accept it. The doctors call this graft rejection.
If the corneal transplant becomes cloudy it is still possible to repeat the operation several times. If all operations fail, one can try a less common operation, odontokeratoprosthesis. There have been many articles describing this tooth-into-the-eye-operation. A thin slice of a tooth is used, not the whole tooth. A clear plastic lens is placed in the root canal in the middle of the tooth slice. The thin piece of tooth is then sewn over a very small corneal opening and covered with mucous membrane. Once the operated eye has healed, a small opening is made in the mucous membrane covering the clear lens and light can then enter through the lens into the eye. These operations are rare.
Iris and Ciliary body
Iris is the colored ring in the front part of the eye. It is a thin layer of fine muscles. In its center is a hole, the pupil. Light passes through the pupil into the eye. The pupil becomes small (constricts) in bright light and larger in dim light.
The ciliary body is located just behind the iris. The lens is attached to the ciliary body by very thin thread-like structures. The surface of the ciliary body secretes clear fluid that circulates through the pupil into the anterior chamber and out of the anterior chamber via chamber angle. The anterior chamber angle is the place where the iris and the cornea meet (see Figure 11).
Lens
The lens of the eye is a small, clear disc. It is very dry. It contains only 65% water. A young person's lens is pliable (flexible). It can change form by becoming thicker or thinner. When it is thin the person sees far, when it is thick he sees at near distance. That is why a young person can see clearly both at near and far. As we become older the lens becomes larger and harder and can no longer change its form as easily as before. That is why we need reading glasses for focusing at near when we get older.
The lens can become cloudy. Cataract is a cloudy lens.
Vitreous body
Vitreous is thick, jelly-like fluid behind the lens. This jelly contains thin threads and small particles that we usually cannot see.
|
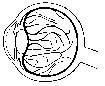
Fig.3. Vitreous body contains microscopically thin threads |
Sometimes, however, the thin threads, (vitreous floaters) become visible in the image that we see. For example, we may see them when we look at the clear sky or white snow. It may look as if there were threads or a fine network floating in the air. If you move your eyes quickly, the threads move in front of the image. The vitreous floaters come and go; they can disappear for years and then appear again. If they are unchanged there is no reason for worry. However, if new floaters appear, the eyes should be examined by an ophthalmologist.
During normal aging, the thin supporting threads of the vitreous become detached from the surface of the retina. Sometimes a small piece of retina may become detached with a thread. The small hole in the retina most often heals and needs no treatment but sometimes it has to be sealed back in place by a ring of laser burns. The laser burns seal the edges of the retinal hole and prevent retinal detachment from developing.
Retina
The retina is a thin, transparent membrane surrounding the vitreous body. It is the part of the eye that actually sees. Light is absorbed by the sensory cells in the outer layers of the retina. There are two kinds of sensory cells, cones and rods. Cones function best in daylight, rods in twilight and dark. We see colors through cone function. Rods do not react to different colors. They see only different shades of grey. That is why we do not see colors when the dusk becomes sufficiently dark.
 A A
|
 B B
|
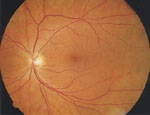
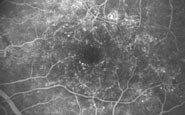
Figure 3a. A. Normal retina as it is seen through the pupil and in the photographs taken through the eye. The artery of the retina enters into it through the optic disc and the vein leaves the retina through it. There is a network of minute capillaries between the arterial and the venous side of the branching vessels. They are visible in fluorescein angiograms. B. Fluorescein angiogram of a retina with diabetic changes in the capillaries, widening of the capillaries and microaneurysms. Note that there are no capillaries in the very centre of the retina, in the fovea.
Retinal blood vessels are very thin vessels. They can be affected by many diseases. Physicians look into the eye to see the retina and the retinal vessels. The "eye grounds" (i.e. the retinas) are checked particularly often in patients who have diabetes or high blood pressure.
The small lamp that the physicians use to see the eyeground is called ophthalmoscope. If the front part of the retina has to be seen, the ophthalmologist uses an indirect ophthalmoscope, a light fixed on spectacles or in a head band and a lens in his/her hand. (S)he may also use slit-lamp (special microscope) and a contact lens (three-mirror- lens) on the cornea (Fig.18) or a lens held in front of the eye.
Choroid
Choroid is a thin layer of vessels behind the retina. The outer layers of the retina get their nutrition from the choroidal circulation. The very central part of the retina, the macula also gets its nutrition from the choroidal circulation.